Medical ophthalmology is an holistic specialty which provides specific expertise in the diagnosis and medical treatment of people with disorders of vision.
More than 50% of new ophthalmic referrals present with a medical rather than surgical problem; hence medicine comprises a large proportion of the workload of any eye department.
Entry to medical ophthalmology training is from either internal medicine/ core medical training or ophthalmology specialty training.
Medical ophthalmology - trainee characteristics
Trainee physicians with the skills detailed below will be suited to a training programme in medical ophthalmology:
-
good team-player skills, including skills in clinical leadership and change-management
-
flexibility, attention-to-detail and lateral thinking
-
excellent communication skills - both spoken and written
-
the ability to work (and enjoy working) under pressure.
Working in medical ophthalmology
The specialty
Medical ophthalmology is an emerging medical specialty in the United Kingdom. In the future it is expected there will be one ophthalmic physician (medical ophthalmologist) per population of 263,000.
The primary purpose of the specialty is the medical assessment, investigation, diagnosis and management of disorders affecting vision, particularly:
-
inflammatory disorders affecting vision (eg uveitis, scleritis, corneal graft rejection, systemic vasculitis
-
vascular disorders affecting vision (eg diabetes, arteriosclerosis, hypertension, stroke)
-
neurological disorders affecting vision (eg multiple sclerosis, stroke, pituitary disorders, thyroid eye disease)
-
public visual health (eg diabetic retinopathy screening).
Other important aspects include:
-
genetic disorders affecting vision (eg retinitis pigmentosa)
-
retina-specific disorders affecting vision (eg age-related macular degeneration)
-
visual rehabilitation (eg age-related macular degeneration)
-
ophthalmic procedures, particularly laser therapy for diabetic retinopathy, and local injection therapy for age-related macular degeneration.
Application of medicine in ophthalmology
Of the new referrals to ophthalmology that require intervention or specialist follow-up, 50% are medical in nature and benefit from the expertise of a clinician with expertise in internal medicine.
New medical treatments for eye disease, including the use of biological agents for inflammatory eye disease, have increased the demand for medical specialists in ophthalmology.
The Centre for Workforce Intelligence issued a report in 2014 recommending a staged increase in medical ophthalmology training posts to meet the growing requirement for medical care in ophthalmology.
Application of ophthalmology in medical specialties
Expertise in ophthalmic medicine is also appropriate for diabetes where the prevalence is expected to rise by 60% in the next decade as a consequence of the ageing population and the epidemic of obesity.
As the eye is a direct extension of the brain, then expertise in neurology is beneficial as many patients with visual disorders have conditions affecting the brain and its pathways rather than the eye itself.
The ophthalmic physician requires to have varied clinical skills beyond expertise in the assessment and diagnosis of visual symptoms and signs. He or she must have expertise in immunosuppression, neurology and cardiology.
In addition, many ophthalmic physicians will be involved in managing large diabetic retinopathy screening programmes, which require organisational and public health skills. Some will be required to manage retina-specific disorders requiring practical skills such as laser therapy and intra-ocular injections.
Benefits and workload
Ophthalmic medicine is a fascinating and rewarding specialty. It is predominantly out-patient based.
The workload of an ophthalmic physician is varied ranging from the personal delivery of care such as laser therapy for diabetic retinopathy through to the intellectual challenge of neuro-ophthalmic disorders. It is also very rewarding with the majority of conditions responsive to therapy. There are opportunities to specialize within medical ophthalmology and to combine clinical care with research or educational roles.
Further information
General / application queries
For general queries relating to areas such as eligibility criteria, making an application or the Oriel system, please contact the Physician Specialty Recruitment Office.
Queries regarding the progress of a submitted application should be directed to the lead recruiter for this specialty. The lead recruiter for medical ophthalmology is South West Severn Recruitment:
| NHS England South West - Severn | ||||||
|---|---|---|---|---|---|---|
| Postal address | Level 1 Park House 1200 Parkway Newbrick Road Bristol Parkway North Stoke Gifford Bristol BS34 8YU |
|||||
| email address | [email protected] | |||||
| website | www.severndeanery.nhs.uk |
|||||
Group 2
This is a Group 2 specialty and requires completion of the first two years of the internal medicine training (IMT) stage 1 programme or equivalent. Please visit the am I eligible? section of this website for further information about the eligibility criteria for Group 2 specialties.
Please be aware that this specialty accepts applicants from Ophthalmology training routes, in addition to core-level physician training.
Non-physician applicants must have obtained the basic specialty professional examination in addition to specific clinical experience and competences to be eligible.
Please view the specialty's person specification for information about the requirements for applying from a non-physician background and the deadlines for when this must be achieved.
Commitment to specialty
The specialty will not be assessing your commitment to specialty as part of the shortlisting process and will score your application purely via the self-assessment scoring framework. Commitment to specialty will be assessed as part of the interview.
As part of the process of applying to HST, you may wish to gain an idea of how recruitment progressed in previous years for the various specialties participating in the nationally-coordinated recruitment.
To this end, we have published data dating back to 2013 (where this is available), based around four main areas:
-
Competition ratios - application numbers submitted to each specialty, along with the number of NTN and LAT posts available in each. It is worth noting that posts are subject to change throughout the round (increasing on average between 20-40%), and post numbers for this data are taken at the end of the round.
-
Shortlist scores - the scores awarded to all submitted applications, including average scores and distribution nationally.
-
Total scores - the total score awarded to all candidates who completed the full recruitment process for a specialty (application and interview), including some analysis of scores.
-
Post fill rates - the number of posts filled by region.
We have published information for all specialties participating in our process that year; consequently not all specialties will have data in all cases.
Round 1
| Year | Apps. | NTN posts | LAT posts | Total posts | Comp. | Unique* |
|---|---|---|---|---|---|---|
| 2023 | 15 | 5 | 0 | 5 | 3 | 47% |
| 2022 | 6 | 6 | 0 | 6 | 1 | 33% |
| 2021 | 21 | 4 | 0 | 4 | 5.2 | N/A |
| 2020 | 7 | 3 | 0 | 3 | 2.3 | 57% |
| 2019 | 12 | 7 | 0 | 7 | 1.7 | 50% |
| 2018 | 4 | 3 | 0 | 3 | 1.3 | 50% |
| 2017 | 10 | 4 | 0 | 4 | 2.5 | 70% |
| 2016 | 9 | 1 | 0 | 1 | 9.0 | 44% |
| 2015 | 9 | 5 | 0 | 5 | 1.8 | 44% |
* the percentage of unique candidates that only applied to this specialty (out of the PSRO-coordinated specialties)
Medical ophthalmology has not participated in round 2 in these years.
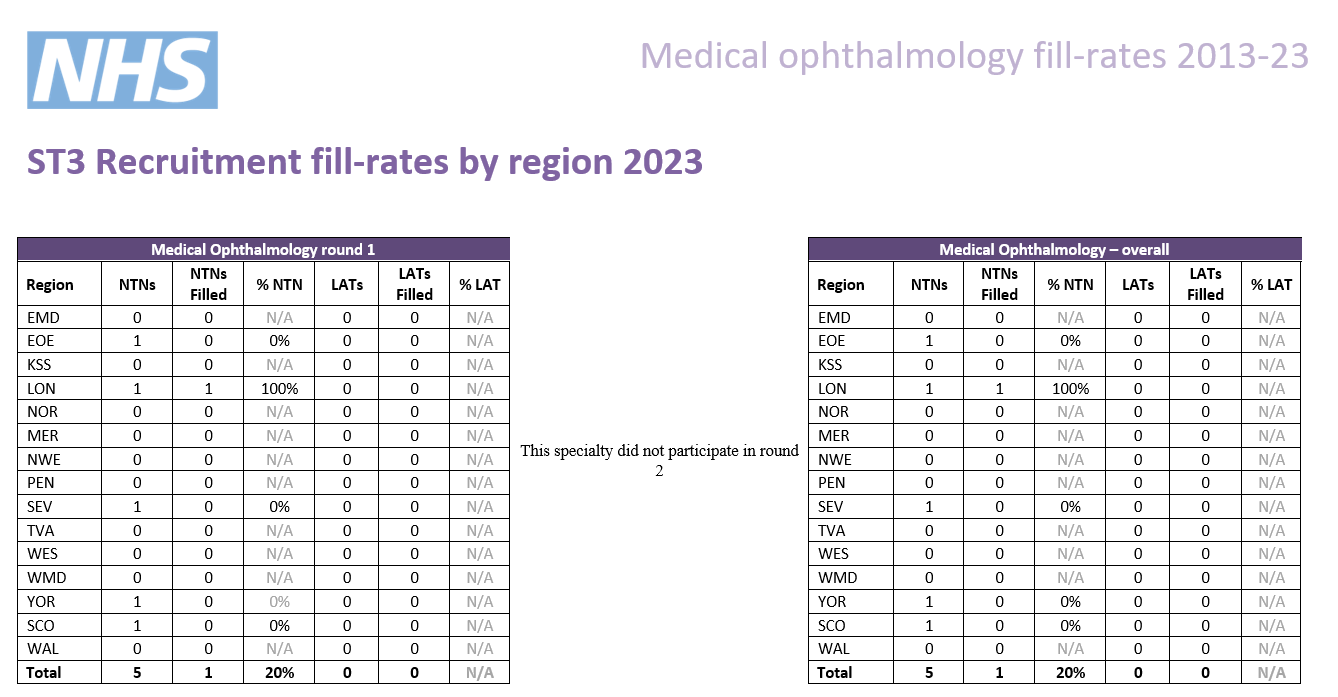
Indicative post numbers
Indicative vacancy numbers are available in the table below, broken down by region and divided between substantive national training number (NTN) and locum appointment for training (LAT) posts. In many cases these will be presented as a range (e.g. 1-4) as it is not always possible for regions to know at this stage how many vacancies there will be.
It is the intention that indicative post numbers for all regions will be published prior to the application opening date, although this cannot be guaranteed. Please note that this table is not likely to be updated subsequent to indicative numbers and actual numbers will be confirmed when programme preferences are opened later in the round.
Numbers subject to change
Please be aware that it is not uncommon for vacancy numbers to change as the round progresses.
More commonly, post vacancy numbers can increase as the round goes on (and confirmation of posts becomes available); but it is also possible that numbers can reduce as well. In the past, post numbers have risen an average of 20-40% from the start to the finish of the round but this can vary greatly for individual specialty/region combinations.
It is possible that regions which do not have a post at the start of the round may declare one after applications have closed. Whilst we try and minimise instances of this, it is not always possible to predict vacancies so even if there appears not to be a vacancy in your preferred specialty/region combination, you may wish to consider applying in case one becomes available during the round; you can check with the region concerned if you wish to check on the likelihood of a post arising.
Generally, once a region enter a post into a round they would always have at least one post available and would only withdraw it in exceptional circumstances.
Round 1 Interview dates & posts
|
Region
|
NTN posts
|
LAT posts*
|
Evidence upload date(s) | Interview date(s) |
|---|---|---|---|---|
|
East Midlands
|
0 | N/A |
18/12/23 - 05/01/24
|
18 March 2024 |
|
East of England
|
1 | N/A | ||
|
London
|
0 - 1 | N/A | ||
|
Kent, Surrey and Sussex
|
0 | N/A | ||
|
North East
|
TBC | N/A | ||
|
North West
|
0 - 1 | N/A | ||
|
South West - Severn
|
0 - 1
|
N/A | ||
|
Thames Valley
|
TBC | N/A | ||
|
Wessex
|
TBC | N/A | ||
|
West Midlands
|
0 - 2 | N/A | ||
|
Yorkshire & Humber
|
TBC | N/A | ||
|
Scotland**
|
1 |
TBC
|
||
|
Wales
|
TBC |
TBC
|
*English LATs
Please note, English regions do not recruit to LAT posts.
**Scotland post numbers
If you are interested in working in Scotland, a breakdown of post numbers by the four Scottish regions is available on the Scottish Medical Training website. This has details of all specialty training post numbers in Scotland, including specialties which are not part of the nationally-coordinated process.
The SMT website will always be the more accurate one where they differ.
Interview content
The interview be split across two separate stations with a separate pair of interviewers scoring you on the areas within their station. There will be four questions between 5-10 minutes in length. You will be marked on these questions, giving four scored areas in total. The headings below show the question areas and in which station they will be covered, along with information about what will be assessed.
Each station will last 15 minutes, so including the time between stations, the interview will be approximately 35-40 minutes.
Please note that this is subject to change and will be confirmed by the date of interview.
Prior to this question you will be given a clinical scenario and a short while to review it. You will then be asked questions relating to this scenario. This question will last approximately 10 minutes.
The clinical scenario will be relatively brief (a few sentences), so once you have seen this, the remainder of the preparation time will allow you to undertake some short mental preparation. Whilst it is permitted to make notes, these must be destroyed as soon as your interview is completed and not shared with anyone.
Clinical scenario considerations
The scenario will describe a hypothetical clinical situation which has arisen in which you are, or have become, involved. Some points to consider when reviewing the scenario and preparing for discussion are:
- what steps you would take
- any potential treatments possible
- any further information you would gather
- how you would go about communicating with any people (eg patients, family members, colleagues) involved in the scenario
You should also consider any other factors you deem appropriate, using your experience and professional judgement.
This question will be a discussion of professionalism and governance.
This discussion will be prompted by a short question (often a single sentence) provided by interviewers. This will not be given to you before - this will be given verbally by interviewers once the previous question is finished. This question will last approximately 5 minutes.
This section of the interview is designed to assess your demonstration and understanding of professionalism and governance in a given situation.
Familiarise yourself with Good Medical Practice
Please note - assessment of professionalism & governance is underpinned by the principles of GMC Good Medical Practice.
This question will see you given an ethical scenario to review. As with the clinical scenario, this takes the form of a hypothetical situation, described briefly in text form, details of which will be given to you before discussion. You will have a short while to review the scenario and there will be approximately 5 minutes of discussion afterwards.
This scenario focuses less on a clinical situation, and deals more with consideration of the moral, ethical, legal (etc.) issues which may arise in a situation.
The area of assessment here will be your suggested responses to the ethical scenario during discussion, as well as your knowledge of the different considerations required.
This question will focus on your suitability for and commitment to training in the specialty and give you opportunity to expand on the information provided in your application form.
This question will last approximately 10 minutes.
Scoring framework
The score of 1-5 an interviewer will award you for each assessment area is judged in relation to how well you perform against an expected level. Below is the framework used to award scores at interview, as well as interpretation of what these scores represent:
|
Mark
|
Rating
|
Assessment
|
|
1 |
poor |
not considered appointable |
|
2 |
area for concern |
performed below the level expected from a core level trainee applying to the specialty; |
|
3 |
satisfactory |
performed at the level expected of a core level trainee applying to the specialty; |
|
4 |
good |
above average ability; |
|
5 |
excellent |
highly performing trainee; |
As shown in the table, for each of the question areas at interview, 3/5 is considered a satisfactory score; and reflects the level of performance that would be expected of a trainee ready to progress to a specialty training programme.
Should your performance go above and beyond this expected level, interviewers can award marks of 4/5 or 5/5 as appropriate.
Conversely, should your interview performance not reach the expected level, then interviewers can award marks of 1/5 or 2/5, as reflects their level of concern over your performance.
Appointability
Raw interview score (RIS)
The RIS is the sum of all eight scores awarded to you during your interview, but before any weighting is applied.
As each individual score will be between 1 and 5, your RIS will be between 8 and 40.
Appointability requirements
To be classed as 'appointable', you must meet all three criteria below:
- none of your eight interview scores can be 1/5
- no more than two of your eight interview scores can be 2/5
- your RIS must be 24 or above.
If you meet all three requirements, your application will be assessed as appointable, and can progress to be considered for post offers.
However, if you fail to meet any of these requirements, your application must then be assessed as not appointable, and it will progress no further in that round.
Total score
After interview, a weighting is applied to the scores in each area, as well as your application score.
These scores are then combined to give your total score which determines your ranking, which will in turn be used to inform how offers are made. The weighting of different sections, as well as the method by which your total score is established, is detailed in the table accessible through the link below:
|
|
Interviewer 1
|
Interviewer 2
|
Weighting
|
Max score
|
|
Question 1 |
||||
|
Clinical scenario |
/ 5 |
/ 5 |
2.5 |
25 |
|
Question 2 |
||||
|
Professionalism and governance |
/ 5 |
/ 5 |
1.2 |
12 |
|
Question 3 |
|
|
|
|
|
Ethical scenario |
/ 5 |
/ 5 |
1.8 |
18 |
|
Question 4 |
||||
|
Suitability and commitment |
/ 5 |
/ 5 |
2.5 |
25 |
|
Raw interview score |
/ 40 |
|||
|
Interview score (w weighting) |
/ 80 |
|||
|
Application score |
/ 50 |
0.4 |
/ 20 |
|
|
Total score |
/ 100
|
|||